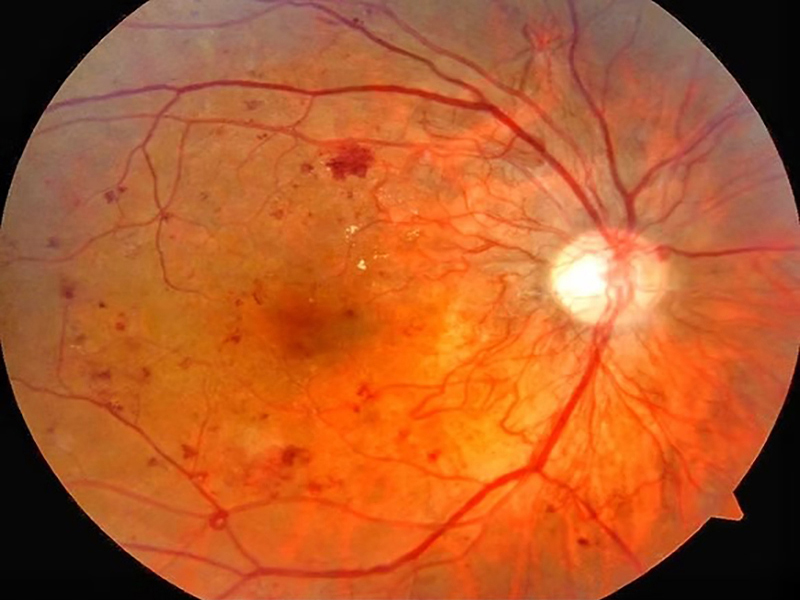
Diabetic retinopathy is a progressive eye disease that affects individuals with diabetes, leading to potential vision impairment or blindness if left untreated. It occurs due to damage to the retinal blood vessels caused by prolonged elevated blood glucose levels. Early detection, routine monitoring, and appropriate medical intervention can significantly mitigate the risk of severe complications.
Pathophysiology and Risk Factors
Diabetic retinopathy results from chronic hyperglycemia (increased blood sugar), which leads to structural and functional abnormalities in the retinal vasculature. The excessive glucose levels cause endothelial dysfunction, inflammation, and oxidative stress, leading to capillary occlusion and leakage. Over time, this vascular damage compromises the oxygen supply to retinal tissues, triggering the release of vascular endothelial growth factor (VEGF), which promotes abnormal blood vessel growth.
Key risk factors for diabetic retinopathy include:
-
Duration of Diabetes: The likelihood of developing diabetic retinopathy increases with the duration of diabetes, particularly after 10 years or more.
-
Poor Glycemic Control: Chronic hyperglycemia accelerates retinal damage, emphasizing the importance of consistent blood sugar regulation.
-
Hypertension and Dyslipidemia: Elevated blood pressure and cholesterol contribute to vascular damage, exacerbating retinal changes.
-
Pregnancy:Expectant mothers with diabetes may experience a rapid progression of retinopathy due to hormonal changes and increased metabolic demands.
-
Smoking and Sedentary Lifestyle: Tobacco use and physical inactivity further impair vascular health, elevating the risk of diabetic retinopathy.
Clinical Stages of Diabetic Retinopathy
Diabetic retinopathy is categorized into distinct stages based on the severity of retinal damage:
-
Mild Nonproliferative Diabetic Retinopathy (NPDR): Characterized by microaneurysms, which are small bulges in the retinal capillaries that may leak fluid or blood.
-
Moderate NPDR: Blockages in some retinal blood vessels occur, reducing blood flow and leading to retinal ischemia and increased leakage.
-
Severe NPDR: A significant number of retinal vessels become occluded, depriving retinal areas of oxygen. This leads to an increased release of VEGF, heightening the risk of disease progression.
-
Proliferative Diabetic Retinopathy (PDR): The most advanced stage, marked by the proliferation of abnormal new blood vessels (neovascularization), which can rupture and cause vitreous hemorrhage or retinal detachment, leading to severe vision loss.
Symptoms and Clinical Manifestations
Diabetic retinopathy may remain asymptomatic in its early stages, necessitating regular screening. As the disease progresses, patients may experience:
-
Blurred or fluctuating vision
-
Increased number of floaters or dark spots
-
Impaired night vision
-
Partial or complete loss of vision in severe cases
Diagnostic Evaluation
Early diagnosis through comprehensive ophthalmologic examinations is crucial for effective management. Diagnostic modalities include:
-
Dilated Fundus Examination: Performed by an ophthalmologist to assess retinal abnormalities such as hemorrhages, microaneurysms, and neovascularization.
-
Optical Coherence Tomography (OCT): Provides cross-sectional imaging of the retina to evaluate retinal thickness and detect macular edema.
-
Fluorescein Angiography: A dye-based imaging test that highlights retinal blood flow abnormalities, capillary leakage, and areas of ischemia.
Management and Treatment Strategies
The primary goal of treatment is to prevent disease progression and preserve vision through meticulous glycemic control and medical interventions.
Glycemic and Cardiovascular Risk Management
-
Tight Blood Sugar Control: Maintaining HbA1c levels below 7% significantly reduces the risk of retinopathy progression.
-
Blood Pressure and Lipid Management: Using antihypertensive medications and statins can minimize vascular damage and protect retinal health.
Medical and Surgical Interventions
-
Laser Photocoagulation Therapy: A focal or panretinal laser treatment that seals leaking blood vessels and prevents further abnormal vessel growth.
-
Intravitreal Anti-VEGF Injections: Medications such as ranibizumab, aflibercept, or bevacizumab are injected into the vitreous cavity to inhibit VEGF, reducing neovascularization and macular edema.
-
Vitrectomy: A surgical procedure performed in advanced cases to remove vitreous hemorrhage or repair retinal detachment.
Preventive Measures and Lifestyle Modifications
Preventing diabetic retinopathy requires a multidisciplinary approach, emphasizing:
-
Regular Ophthalmologic Examinations: Annual eye exams with pupil dilation for early detection.
-
Dietary and Exercise Modifications: A nutrient-rich diet and regular physical activity support glycemic and cardiovascular health.
-
Smoking Cessation: Eliminating tobacco use reduces oxidative stress and vascular damage.
Conclusion
Diabetic retinopathy remains a leading cause of preventable blindness among individuals with diabetes. Through proactive disease management, regular screening, and timely medical intervention, the risk of vision loss can be significantly reduced. Patients should work closely with their healthcare providers to optimize diabetes management and undergo routine eye evaluations to safeguard their visual health.