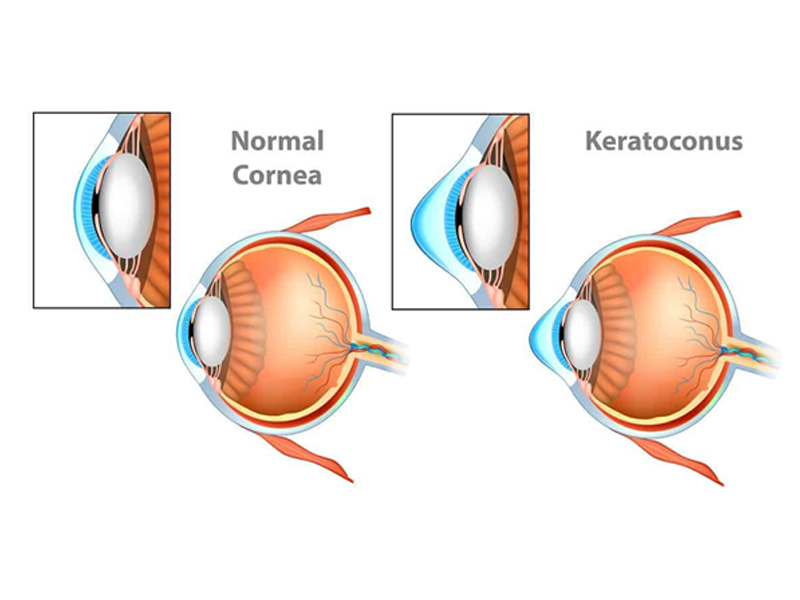
Understanding Keratoconus
Keratoconus is a progressive eye disorder in which the normally round cornea (the transparent front part of the eye) thins and gradually bulges outward into a cone shape. This irregular shape prevents light from being focused correctly onto the retina, leading to blurry and distorted vision. The condition often starts during puberty or early adulthood and can progress over several years.
Causes and Risk Factors
While the exact cause of keratoconus is not completely understood, it is believed to be due to a combination of genetic, environmental, and biochemical factors. Some key contributors include:
-
Genetics: Individuals with a family history of keratoconus have a higher risk of developing the condition, suggesting a hereditary component.
-
Eye Rubbing: Chronic eye rubbing, especially in individuals with allergies or atopic conditions, has been associated with the progression of keratoconus. It can weaken the corneal structure over time.
-
Underlying Medical Conditions: Certain conditions, such as Down syndrome, Ehlers-Danlos syndrome, Marfan syndrome, asthma, and retinitis pigmentosa, have been linked to an increased risk of keratoconus.
-
Environmental Factors: Long-term exposure to ultraviolet (UV) radiation, oxidative stress, and improper contact lens wear may contribute to corneal degeneration.
-
Hormonal Influences: Some researchers suggest that hormonal changes during puberty or pregnancy may play a role in the development or progression of keratoconus.
Symptoms of Keratoconus
Symptoms of keratoconus often start in adolescence or early adulthood and may worsen over time. Common symptoms include:
-
Blurred or distorted vision: Due to irregularities in the corneal shape, light does not focus properly, leading to wavy or double vision.
-
Frequent changes in prescription: People with keratoconus may find that their glasses or contact lens prescription changes frequently.
-
Increased sensitivity to light and glare: Bright lights may cause discomfort, making night driving particularly challenging.
-
Difficulty seeing at night: Night vision impairment is common in keratoconus patients.
-
Halos or ghosting around lights: Objects may appear with a shadowed or duplicated effect.
-
Eye strain or discomfort: Some individuals may experience eye irritation, fatigue, or headaches due to poor vision.
-
Sudden worsening of vision: In rare cases, sudden corneal swelling (hydrops) can occur, leading to a rapid decline in vision and discomfort.
Diagnosis
Keratoconus is diagnosed through a comprehensive eye examination, which may include the following tests:
-
Slit-Lamp Examination: A microscope is used to examine the cornea for signs of thinning, scarring, and other abnormalities.
-
Corneal Topography: A computerized imaging technique that maps the shape of the cornea, helping to detect irregularities and track progression.
-
Pachymetry: A test that measures corneal thickness, which is crucial in identifying early-stage keratoconus.
-
Keratometry: Measures the curvature of the cornea to detect steepening associated with keratoconus.
-
Wavefront Analysis: Evaluates visual distortions caused by corneal irregularities.
Treatment Options
Treatment for keratoconus depends on the severity of the condition and how much it is affecting vision. Early detection and management can slow progression and improve visual function.
Non-Surgical Treatments
-
Glasses and Soft Contact Lenses: In the early stages, prescription glasses or soft contact lenses may be sufficient to correct vision.
-
Rigid Gas Permeable (RGP) Lenses: These lenses provide a smoother refractive surface by vaulting over the irregular cornea, improving vision.
-
Hybrid Lenses: These lenses combine a rigid center with a soft outer ring for improved comfort and vision.
-
Scleral Lenses: Larger than traditional contact lenses, scleral lenses rest on the sclera (white part of the eye) and create a smooth optical surface.
-
Corneal Cross-Linking (CXL): A minimally invasive procedure that strengthens the cornea using ultraviolet (UV) light and riboflavin drops. This helps halt the progression of keratoconus and may prevent the need for more invasive treatments.
Surgical Treatments
-
Intrastromal Corneal Ring Segments (ICRS): Small, semi-circular implants are inserted into the cornea to reshape it and improve vision.
-
Topography-Guided Photorefractive Keratectomy (TG-PRK): A laser procedure that reshapes the cornea and may be used in combination with cross-linking.
-
Corneal Transplant (Keratoplasty): In advanced cases where vision cannot be corrected with lenses or other treatments, a partial (Deep Anterior Lamellar Keratoplasty, DALK) or full-thickness (Penetrating Keratoplasty, PK) corneal transplant may be necessary.
Living with Keratoconus
Managing keratoconus requires regular eye care and lifestyle adjustments. Here are some tips:
-
Regular Eye Checkups: Routine monitoring helps track disease progression and ensures timely treatment.
-
Avoid Eye Rubbing: Reducing mechanical stress on the cornea can prevent worsening of the condition.
-
Wear UV-Protective Sunglasses: Shielding your eyes from UV rays can help slow corneal damage.
-
Use Lubricating Eye Drops: These can reduce eye irritation and dryness, improving comfort for contact lens wearers.
-
Proper Contact Lens Hygiene: Follow best practices for cleaning and wearing contact lenses to reduce the risk of infections and complications.
-
Adapt to Visual Challenges: People with keratoconus may benefit from high-contrast screens, anti-glare coatings, and assistive technology for reading or driving.
Prognosis
With early diagnosis and appropriate management, most people with keratoconus can maintain functional vision and a good quality of life. Corneal cross-linking has significantly improved long-term outcomes by slowing or halting progression, reducing the need for corneal transplants. Advances in lens technology and surgical options continue to enhance visual rehabilitation for keratoconus patients.
Conclusion
Keratoconus is a complex but manageable condition. If you experience symptoms such as worsening vision, increased sensitivity to light, or frequent prescription changes, seek an eye examination as early detection can prevent severe vision impairment. With the right treatment plan, individuals with keratoconus can continue to lead active and fulfilling lives. Always follow your doctor’s recommendations for optimal eye health and vision care.